As a charter-boat captain who has ventured offshore for over a thousand trips, I have had to deal with injuries including knife cuts, shark bites, broken bones and profuse bleeding. Aboard a boat, you are farther removed from professional help than when on land. The following tips outline three must-know first-aid techniques.
Profuse Bleeding
Applying direct pressure to the wound is usually the best first step. Sterile gauze packing is preferred, but a clean T-shirt gets the job done. I keep a Tac Pac Pro on board my 228 EdgeWater CC to supplement my primary medical kit, which includes the requisite sterile pressure and packing dressings, tourniquet and more. I also keep sutures, cyanoacrylate super glue and QuikClot in my kit, and have used all of these in emergencies. A tourniquet is a last-ditch measure to stop the bleeding if the other methods are ineffective. Try to elevate the affected body part to slow down the blood loss, and remember to call for help on the VHF or a cellphone and head for the closest landfall.
Broken Bones
Broken bones and/or bad sprains can occur in a variety of ways, from having a hand or finger crushed under a tight anchor line, to slips and falls in rough seas. If a crewmember takes a spill and then can’t put any weight or pressure on a finger, hand or leg, something is probably not right.
According to some of the doctors I fish with, do not attempt to realign a deformed body part or push back a bone that has pierced the skin. Immobilize the affected area above and below the spot with a splint (I normally keep a few paint stirrers on board with duct tape, just in case) and try to pad it with some soft material (like a towel or T-shirt) to reduce discomfort. Head back to the dock.
Quick Tip: All boaters should seek formal first-aid training from organizations such as the (American Red Cross) or the United States Power Squadrons.
Shock
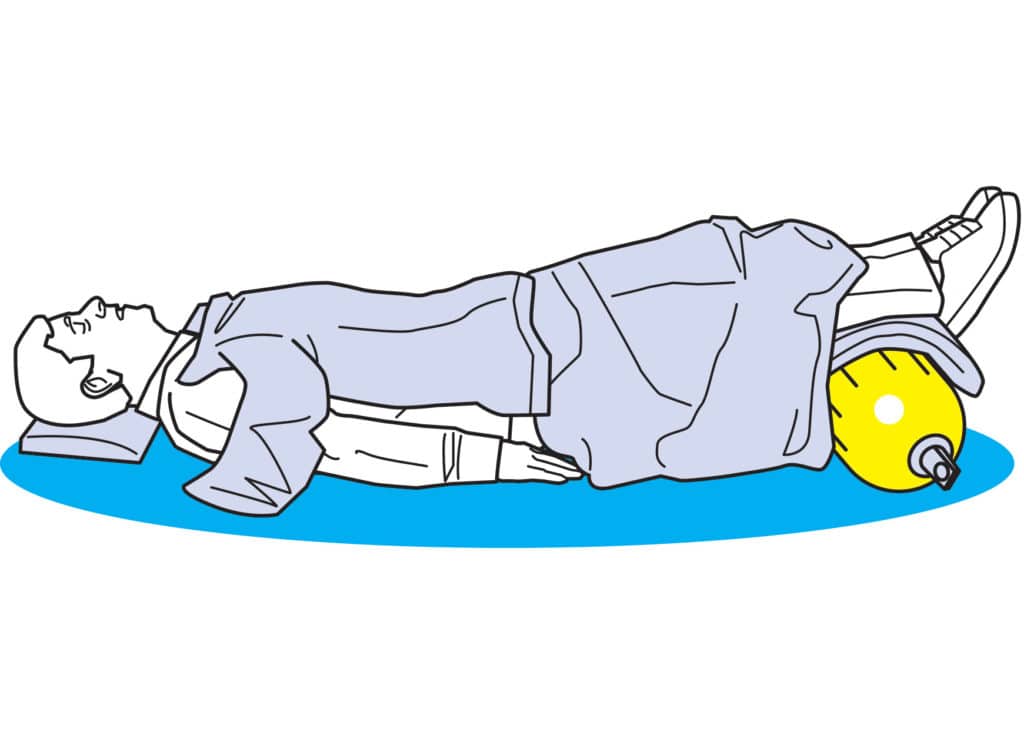
There are several different types of shock and numerous causes. One of the most common forms is hypovolemic shock, which is caused by a sudden and significant loss of blood or body fluids. It’s always considered a life-threatening emergency because if blood volume gets too low, organs won’t be able to keep functioning normally. Symptoms of hypovolemic shock can include rapid heartbeat, weak pulse, extreme weakness or lethargy, dilated pupils, nausea, confusion or disorientation, quick and shallow breathing, and/or cool, clammy skin. If you suspect that someone has gone into shock as a result of an injury, lay them down on the deck on the centerline, elevate their feet by 10 to 12 inches to help direct blood to the vital organs, cover them with a blanket, and monitor their breathing and heart rate for any radical changes. Call for help on the VHF or a cellphone and head back to home port at the best practical speed.









